Out-of-Network Benefits
For the remainder of the summer, we will be reposting educational material on Health Insurance Basics which was originally aired in 2021, with updated 2022 information as appropriate. If you didn’t watch these videos, please do, and tune back in after Labor Day for new material. Thanks, and have a wonderful summer.
Today we feature the Out-of-Network Benefit’s video found at healthcarenavigation.com/
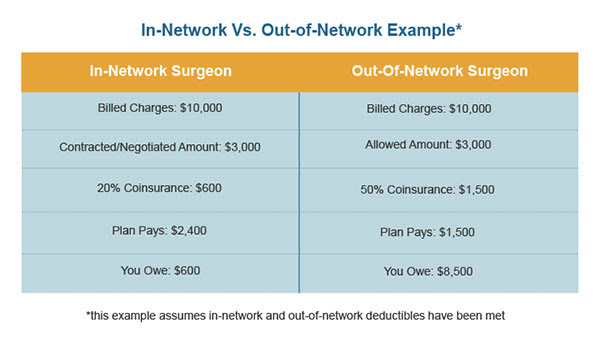
Most of the difficulty stems from consumers thinking their coinsurance amount (the percentage the patient owes) pays for a percentage of billed charges. In reality, the coinsurance percentage is applied only to the insurer’s allowed amount which can be a fraction of billed charges. The example given in the video is of a surgeon who charged $70,000 but the insurer’s allowed amount was $4,600 so the patient’s responsibility was originally $65,825 although ultimately reduced. We have provided an illustration of in-network vs. out-of-network benefits exposure below. With this example patient responsibility for the in-network surgeon is $600 and the out-of-network surgeon $8,500.
Who is to blame for this situation? There is plenty of blame to spread around. Provider charges are often unreasonably high and allowed amounts insurers pay often unreasonably low leaving the uninformed patient vulnerable. In an era where transparency is a buzzword of our time, there is often no transparency in many of these situations.
Federal legislation addressing surprise medical bills took effect in January 2022. That legislation provides some protection in emergency situations or situations where one has surgery scheduled in an in-network hospital with an in-network surgeon and the anesthesiologist is out-of-network.
Our recommendation to everyone who has out-of-network benefits is to become familiar with your out-of-network deductible and out-of-network coinsurance amount. If you then choose to go to an out-of-network provider for a costly procedure like surgery, discuss with the staff in advance what your exposure is and negotiate an acceptable arrangement. You can conduct some research on your own by asking provider office staff for the relevant CPT (Current Procedural Terminology) codes associated with that procedure and researching claims data on fairhealth.org, a major repository of private claims data, using the CPT code information.
For those who’ve already received staggering bills they didn’t expect, respond quickly and in writing inquiring about the charges to the provider. At the same time consider filing an appeal with the insurer.
And for all those who are seeing out-of-network providers whose charges are reasonable and reimbursement from the insurer acceptable, don’t let yourself be lured into thinking that is typical.